I realized that in my Riverview/Essondale post, I mentioned quite a few of the treatments for mental illnesses that they used in the early 20th century, which some people might not know what they entail. In this post I will cover the details on hydrotherapy, insulin shock treatment, metrazol therapy, , electroconvulsive therapy, and lobotomies.
Hydrotherapy
Water was thought to be an effective treatment because it could be heated or cooled to different temperatures, which, when applied to the skin, could produce various reactions throughout the rest of the body. One of the main benefits of hydrotherapy treatment was its ability to take effect quickly. Hydrotherapy could be accomplished with baths, packs, or sprays. Warm continuous baths were used to treat patients suffering from insomnia, those considered to be suicidal and assaultive, and calmed excited and agitated behaviour. A patient could expect a continuous bath treatment to last from several hours to several days, or sometimes even overnight. Bath temperatures typically ranged from 33°C to 38°C, so as not to cause injury to the patients. The bath was often covered by a sheet so that only the patients head wasn’t under water. The patients would sometimes be strapped in so that they couldn’t move and would have to be fed by staff. Packs consisted of sheets dipped in varying temperatures of water, which were then wrapped around the patient for several hours, depending on the case. Sprays functioned like showers, and used either warm or cold water. Cold water was used to treat patients diagnosed with manic-depressive psychoses, and those showing signs of excitement and increased motor activity. Application of cold water slowed down the blood flow to the brain, decreasing mental and physical activity. The temperature for a cold pack ranged between 8°C and 18°C. On few occasions, patients would be cooled down in ice water baths or wrapped in sheets soaked with freezing water.



Insulin Shock Therapy
Insulin shock Therapy, also known as insulin coma therapy, was a form shock therapy in which patients were repeatedly injected with large doses of insulin in order to produce daily comas over several weeks.
Typically, the injections were administered six days a week for about two months, with insulin levels of 150 units, at the point of when comas were produced, at which the dose would be levelled out. After about 50 or 60 comas, the dose of insulin was rapidly reduced before the treatment was stopped; courses of up to two years have been documented.
After the injection patients would experience various symptoms of decreased blood glucose: flushing, pallor, perspiration, salivation, drowsiness or restlessness. If the dose was high enough, stupor and coma would follow. Each coma would last for up to an hour and be terminated by intravenous glucose. Seizures sometimes occurred before or during the coma; many of the patients would be tossing, rolling, moaning, twitching, spasming or thrashing around.
Some psychiatrists regarded seizures as therapeutic and patients were sometimes also given electroconvulsive therapy or metrazol therapy during the coma, or on the day of the week when they didn’t have insulin treatment
The insulin shock therapy mortality rate varied from 1% to 10% of patients treated.



Metrazol Therapy
Metrazol, also known as pentylenetetrazol, corazol, or cardiazol, is a drug formerly used as a circulatory and respiratory stimulant. High doses of the drug cause convulsions, as discovered by the Hungarian-American neurologist and psychiatrist Ladislas Meduna in 1934. Meduna was interested in treating schizophrenia and had made an observation that patients that died with epilepsy had more brain glial cells than patients with schizophrenia. He theorized that by inducing seizures in patients suffering from schizophrenia that it would increase the presence of glial tissue and reverse the mental illness. In other terms, he reasoned that artificially induced epileptic convulsions could be used to cure schizophrenia.
About a minute after the injection, Metrazol produced an explosive. Often these convulsions would result in fractured and broken bones and torn muscles. For the therapy to be effective, it would be given two or three times a week and a typical course of therapy would be thirty to forty injections. Most of the time when the patient regained consciousness they would be confused and cooperative with staff which was seen as a marked improvement. Other times in this odd state the patient would act in a more regressive manner, frightened and scared by the treatment. After a patient received one treatment they were resistant to subsequent treatment, resisting and pleading for it not to be done again and would have to be forcibly treated.
Metrazol therapy was gradually discontinued in the mid 30’s and more commonly replaced with electroconvulsive therapy.

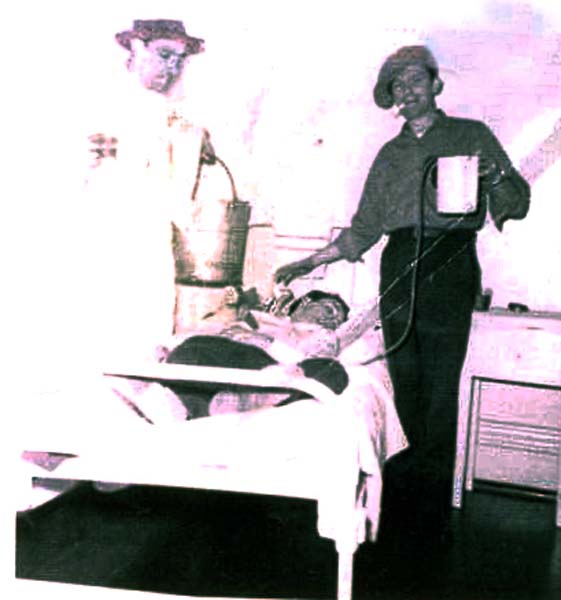

Electroconvulsive Therapy
Italian Professor of neuropsychiatry, Ugo Cerletti, who had been using electric shocks to produce seizures in animal experiments, developed the idea of using electricity as a substitute for metrazol in convulsive therapy and, in 1938, experimented for the first time on a person. Once the trials started on patients, it was found that after 10-20 treatments the results were significant. A positive side effect to the treatment was amnesia. It was because of this side effect that patients could not remember the treatments and had no ill feelings toward it. Electroconvulsive therapy soon replaced metrazol therapy all over the world because it was cheaper, less frightening, less damaging to the patients body and more convenient.
Electroconvulsive therapy was a highly troublesome treatment. There were many examples of ECT being used to subdue and to control patients in psychiatric hospitals. Troublesome patients received several shocks a day, many times without proper restraint or sedation.
ECT was used to treat major depressive disorders, mania, catatonia, and schizophrenia; which it turned out that the therapy actually only helped those patients suffering from depressive disorders. There were many side effects to using electroshock therapy, some of which are effects on memory and effects on the actual structure of the brain.



Lobotomies
Lobotomy is a neurosurgical procedure, a form of psychosurgery, also known as a leukotomy or leucotomy. It consists of cutting or scraping away most of the connections to and from the prefrontal cortex, the anterior part of the frontal lobes of the brain. While some patients experienced symptomatic improvement with the operation, this was achieved at the cost of creating other impairments, and this balance between benefits and risks contributed to the controversial nature of the procedure. Some patients died as a result of the operation and others later committed suicide. Some were left severely brain-damaged. Others were able to leave the hospital, or became more manageable within the hospital.
There were a few different methods of performing a lobotomy. The first procedures involved cutting a hole in the skull and injecting ethanol into the brain to destroy the fibers that connected the frontal lobe to other parts of the brain. The second method introduced a surgical instrument called a leucotome, which contains a loop of wire that, when rotated, creates a circular lesion in the brain. The third method was created because it was much easier and would not require a traditional surgeon and operating room. The technique involved using an instrument called an orbitoclast, a modified ice pick, which the physician would insert through the patient’s eye socket using a hammer. They would then move the instrument side-to-side to separate the frontal lobes from the thalamus, the part of the brain that receives and relays sensory input.



One thought on “Mental Health Treatments”